5255 Longley Ln Reno, NV 89511 775.823.5350 1413 S.Virginia St Reno, NV 89502 775.507.4210 2484 Wingfield Hills Rd C-120 Sparks, Nv 89436 775.993.3640 info@nevPT.com

×
The ACL Project
The Clinic
Philosophy
The Team
Schedule
Blog
Contact
Achilles Tendonitis
ACL Post Surgical Rehab
Ankle & Foot Sprains/Fractures
Degenerative Arthritis/Total Knee Replacement
Frozen Shoulder
Meniscal/Articular Cartilage
Non-Surgical ACL Management
Patellofemoral Syndrome
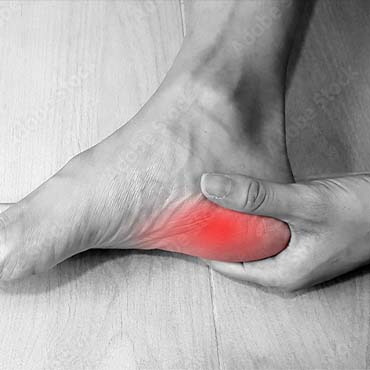
Plantar Fasciitis
Post Surgical Rehabilitation
Rotator Cuff Repair
Shoulder Labral Tears & Instability
Tendinopathy
Throwing Injuries
Total Shoulder Replacement